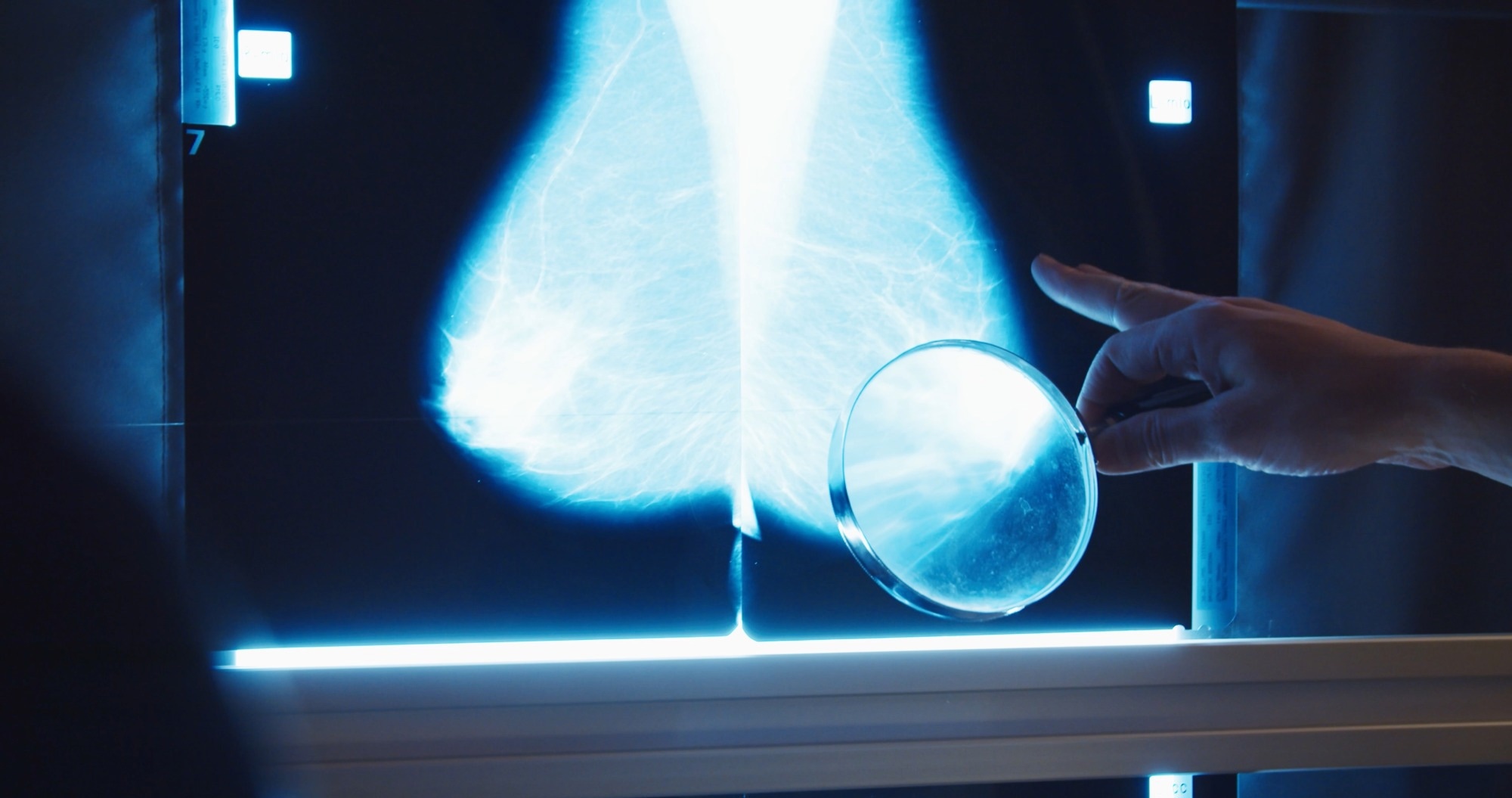
A new study has demonstrated that artificial intelligence (AI) can identify subtle indicators in routine mammograms that may signal an increased risk of developing aggressive breast cancers years before they are diagnosed. Conducted by researchers from the National Health Service (NHS) in the United Kingdom, this large-scale study analyzed the effectiveness of advanced Deep Learning (DL) algorithms in detecting “interval cancers,” which represent a critical gap in current breast cancer screening practices.
The findings, published in the journal npj Digital Medicine, stem from a retrospective validation study involving 112,621 mammogram images. The research focused on four leading DL models, comparing their effectiveness in predicting interval cancers, which comprise approximately 30% of cases diagnosed after a negative mammogram but before the next scheduled screening. These cancers often have more aggressive characteristics, resulting in poorer patient outcomes.
Mirai, an academic model developed by the Massachusetts Institute of Technology (MIT), emerged as the top performer in the study, achieving an interval cancer Area Under the Curve (AUC) score of 0.77. This model flagged about 27.5% of interval cancers by identifying the highest risk among the top 4% of “normal” screening mammogram images.
Understanding the Challenge of Interval Cancers
For years, breast cancer screening protocols have recommended women undergo mammograms every few years, such as every three years in the UK. While these screenings are effective in detecting most breast cancers, they frequently miss interval cancers, which develop between scheduled screenings. These cancers are often more aggressive, leading to worse prognoses and increased mortality rates.
Traditional methods for assessing individual risk have relied on genetic assessments and family history evaluations, which are not routinely implemented in population screening programs. Recent advancements in DL algorithms have led researchers to explore the potential of AI to detect subtle imaging patterns that may elude human radiologists.
The study aimed to fill the knowledge gap by comparing the predictive performance of four advanced DL models: Mirai (MIT), iCAD ProFound AI Risk (commercial model), Transpara Risk (another commercial tool), and Google Health’s Risk Model.
Results and Model Performance
The validation dataset for the study was derived from the UK NHS screening program, consisting of high-resolution “negative” mammograms collected between 2014 and 2017. The researchers monitored participants for five years, observing the development of breast cancers, including interval cancers, during the follow-up period.
The results indicated that Mirai consistently outperformed the other models, achieving a predictive power AUC score of 0.72. The commercial models also demonstrated notable performance, with iCAD scoring 0.70, Google Health at 0.68, and Transpara at 0.65. These scores are significant considering the mammograms had been interpreted as “normal” during routine screenings.
The study highlighted that the DL models could effectively identify women at risk for interval cancers based on initial negative screening results. When researchers analyzed the top 4% of women deemed at highest risk by Mirai, they found that approximately 27.5% of interval cancers in the cohort emerged from this group. Expanding the high-risk category to the top 14% of women doubled the detection rate, capturing around 50.3% of all future interval cancers.
The study also examined the performance of these models across different mammography machine manufacturers. It found that three of the four models performed similarly on images produced by Philips and GE machines. The Transpara model exhibited better performance on GE images compared to Philips, with AUC scores of 0.69 and 0.62, respectively.
Despite these promising results, the authors acknowledged several limitations, including the exclusion of mammograms with implants, incomplete ethnicity data, and the potential for results to not fully generalize across other major mammography systems. They also cautioned that retrospective validation may underestimate the clinical utility of these algorithms, as some cancers might be detected through alternative imaging pathways.
The study’s conclusions suggest that DL models like Mirai can uncover previously unrecognized imaging signals in standard mammograms, providing a pathway to risk-stratified breast cancer screening. The findings pave the way for further investigation into the utility of these tools in prospective clinical trials and real-world screening environments before they are integrated into personalized care protocols.
Future research will be crucial to determine how these AI-driven models can enhance breast cancer screening and ultimately improve patient outcomes.