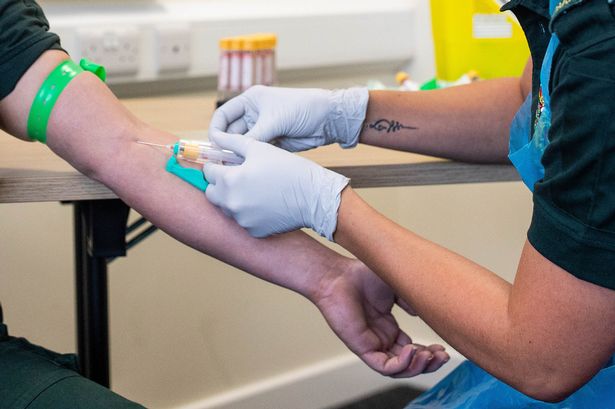
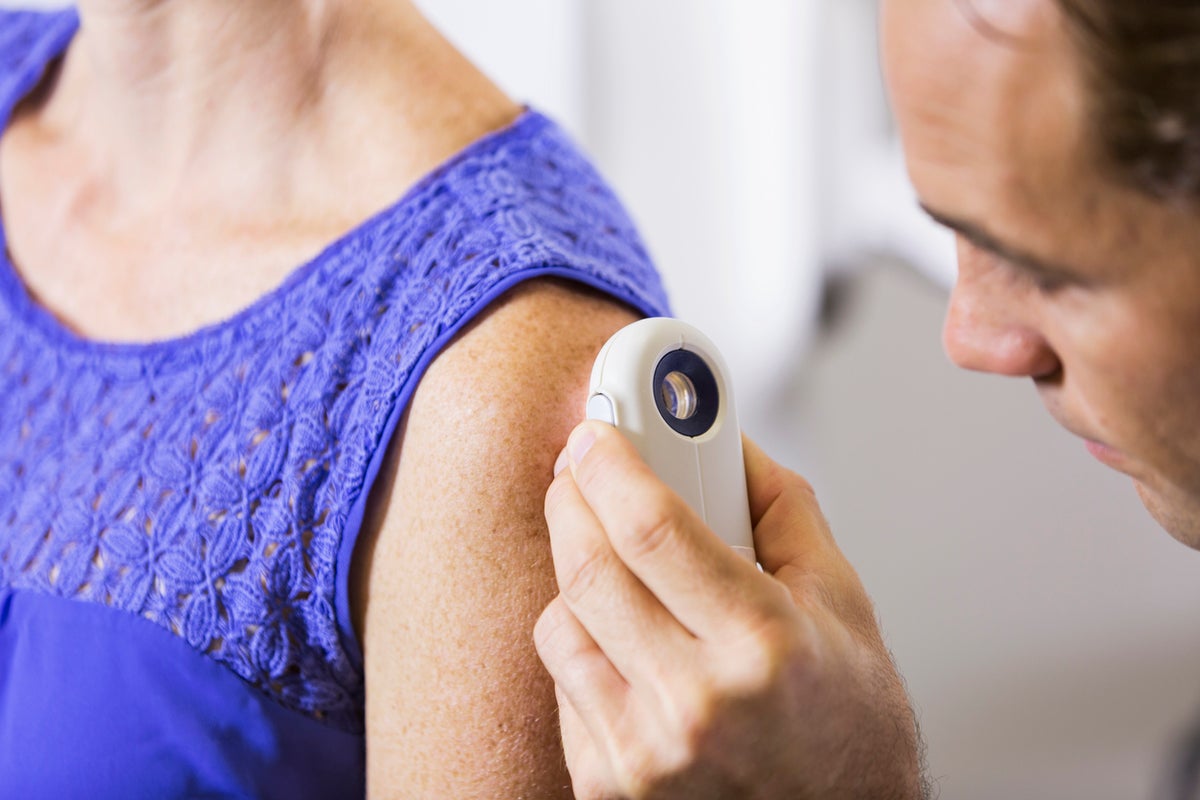
Experts have advised against routine prostate cancer screening for most men in the UK, stating that the potential risks may outweigh the benefits. The UK National Screening Committee (UKNSC) announced its decision, rejecting calls for a population-wide screening program using the prostate-specific antigen (PSA) test. The committee emphasized that indiscriminate screening could cause “more harm than good.”
The UKNSC did recommend a targeted screening program for men with specific genetic risks. This includes men with confirmed BRCA1 and BRCA2 gene variations, who should be screened for prostate cancer every two years starting at age 45. Despite the high incidence of prostate cancer among black men, the committee noted a lack of sufficient data to recommend screening specifically for this group.
The committee’s analysis found that while population-wide screening might lead to a slight reduction in prostate cancer deaths, the high incidence of overdiagnosis presents significant health risks. According to Professor Sir Mike Richards, former national cancer director and chairman of the UKNSC, the modeling indicates that many men diagnosed through such screening might undergo unnecessary treatments for slow-growing or non-threatening tumors. These treatments can lead to serious side effects, including incontinence and erectile dysfunction.
This announcement follows former Prime Minister David Cameron revealing that he had been treated for prostate cancer, prompting renewed calls for screening to be made available to high-risk individuals. Charitable organizations, including Prostate Cancer UK, have long advocated for national screening programs.
Laura Kerby, chief executive of Prostate Cancer UK, expressed disappointment over the committee’s decision, stating, “This will come as a blow to the tens of thousands of men, loved ones, and families who’ve fought for a screening programme.” She emphasized that the committee’s recommendation, while limited, marks a significant step forward in recognizing the need for screening based on genetic factors.
While the committee acknowledged the potential benefit of screening men with BRCA gene variations, it declined to recommend targeted screening for those with a family history of the disease, despite their elevated risk. This has drawn criticism from several health experts who argue that more comprehensive screening could save lives.
Dr. Ian Walker, executive director of policy at Cancer Research UK, noted the positive aspect of the recommendation for men with faulty BRCA genes. He stated, “The UK National Screening Committee’s analysis shows that screening this group will save lives.” However, he reiterated the committee’s position that for other groups of men, current evidence does not support widespread screening.
The future of prostate cancer screening may hinge on ongoing research. Experts are now looking towards the results of the Transform trial, recently launched by Prostate Cancer UK, which aims to investigate whether combining the PSA test with other diagnostic methods, such as rapid MRI scans, can improve screening outcomes. This trial is expected to yield results within two years, potentially informing future recommendations for population-wide screening.
As the conversation around prostate cancer screening continues, the focus remains on balancing the benefits of early detection with the risks of overdiagnosis and unnecessary treatment. The UKNSC’s recent recommendations highlight the need for targeted approaches based on individual risk factors, while ongoing research may pave the way for more effective screening strategies in the future.