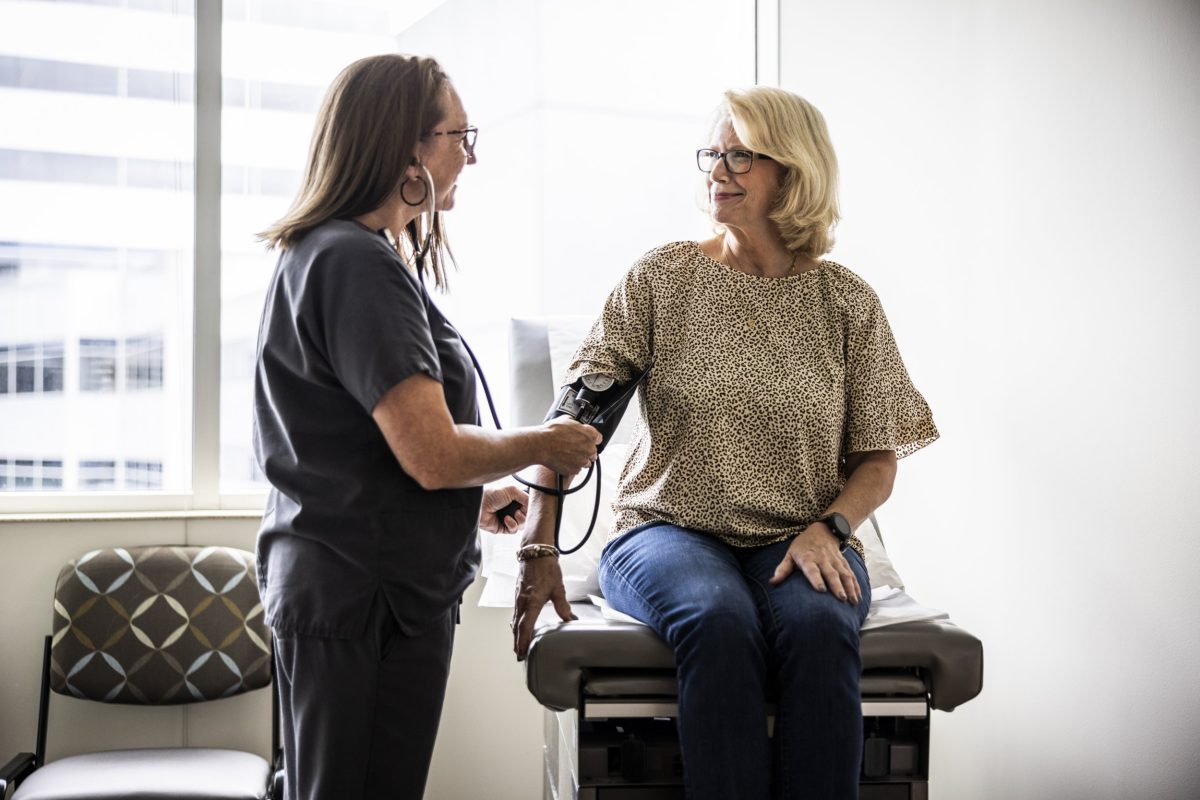
High blood pressure, or hypertension, has become a significant health challenge in the UK, reversing years of progress in its management. Once celebrated as a triumph for the National Health Service (NHS), recent studies indicate that the treatment and identification of this “silent killer” have stalled, particularly since the onset of the Covid-19 pandemic.
Hypertension is a major contributor to heart attacks and strokes, often developing without noticeable symptoms. According to a study published in the journal BMJ Medicine, the improvements the NHS had achieved over the last two decades in diagnosing and treating hypertension have significantly declined. Professor Ian Wilkinson, the president of the British and Irish Hypertension Society, stated, “Hypertension will kill more people in the UK than anything else. But we’ve stalled [on treating it], and we’re going backwards.”
Challenges to Blood Pressure Control
The NHS had previously seen a reduction in the number of undiagnosed hypertension cases and a decrease in average systolic blood pressure. Data from the Health Surveys for England revealed that the percentage of people with undiagnosed high blood pressure fell from 33 percent in 2003 to 24 percent in 2011. Average systolic blood pressure also dropped from 129 mm Hg in 2003 to 124 mm Hg in 2017.
However, between 2017 and 2019, these improvements plateaued. Dr. Ajay Gupta, a consultant in cardiovascular medicine at Queen Mary University of London, attributed this stagnation to unhealthy lifestyle choices, including increased salt consumption and rising obesity rates. A diet high in processed foods has contributed to a resurgence in salt intake, which rose from 7.6 grams per person per day in 2014 to 8.4 grams by 2018, exceeding the recommended maximum of 6 grams.
The Covid-19 pandemic exacerbated existing challenges. During the height of the health crisis, many individuals were discouraged from seeking medical care for non-urgent issues, which resulted in missed opportunities for diagnosis and treatment adjustments. Dr. Gupta noted, “Access to medications, access to evaluations got disrupted. Waiting lists worsened, and the time to see your GP in person worsened. All those things will have a small incremental effect.”
By 2021, the number of individuals with undiagnosed hypertension had increased to 32 percent, with average systolic blood pressure climbing to 126 mm Hg. Preliminary data from 2022 suggests limited improvement in these metrics since the previous year.
The Future of Hypertension Management
The factors contributing to the deterioration of blood pressure control are multifaceted. Professor Wilkinson highlighted the increasing prevalence of overweight individuals as a significant risk factor for hypertension. He indicated that the trend of substituting in-person GP appointments with telephone consultations might also discourage patients from starting necessary blood pressure medications. “If you have a proper conversation about it, you can explain that if you treat this early, and you get the blood pressure to target, they will gain healthy life years,” he said.
The NHS has been approached for comments regarding these findings and ongoing strategies to address hypertension management. As the health crisis evolves, prioritizing the treatment and prevention of high blood pressure will be essential to improving overall public health in the UK.